Exploring the impact of virtual reality on education, surgical planning, and interdisciplinary collaboration for clinicians in head and neck oncology.
https://doi.org/10.1016/j.oraloncology.2025.107444Tumor contouring
Virtual reality enables preoperative tumor contouring, allowing for the precise planning of safety margins. This process involves the accurate delineation of the tumor and surrounding critical structures on imaging, supporting optimized decision-making. Utilizing VR increases the understanding and planning of anatomical areas that require surgical reconstruction.
Through the use of VR technology, multidisciplinary teams can explore the surgical field in a three-dimensional environment, allowing more precise visualization of critical structures and potential radiation exposure zones.
This integrated approach improves margin assessment, strengthens coordination between surgeons and radiation oncologists, and supports informed decision-making that optimizes patient outcomes while minimizing treatment-related complications.
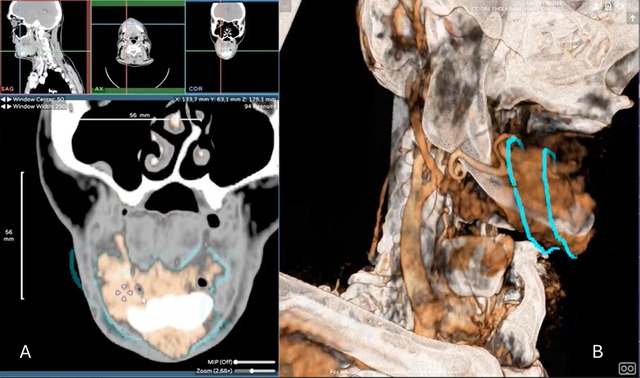
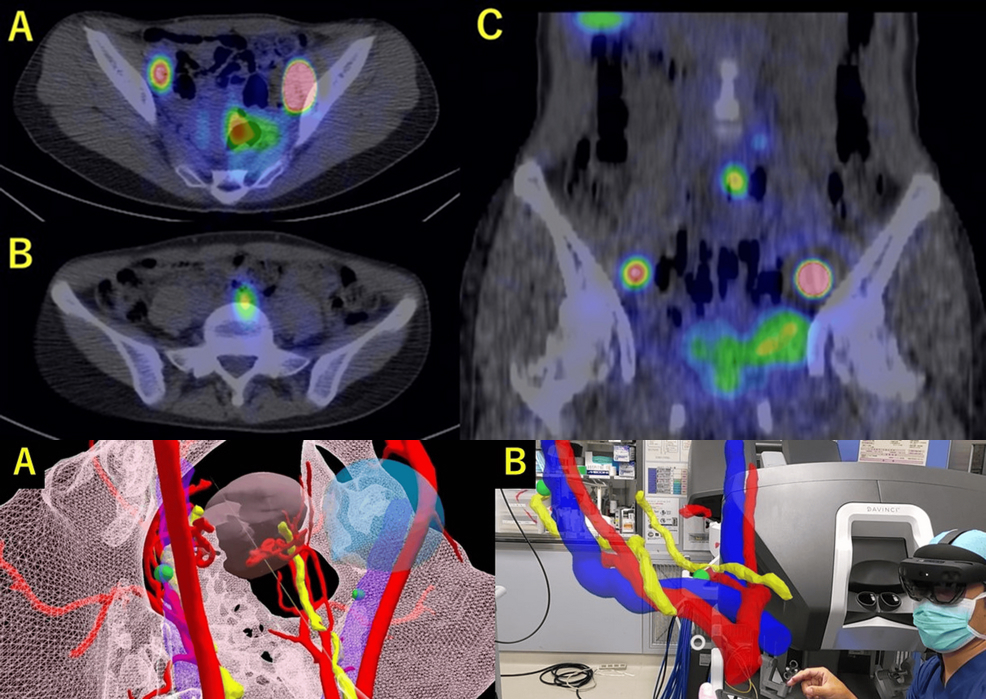
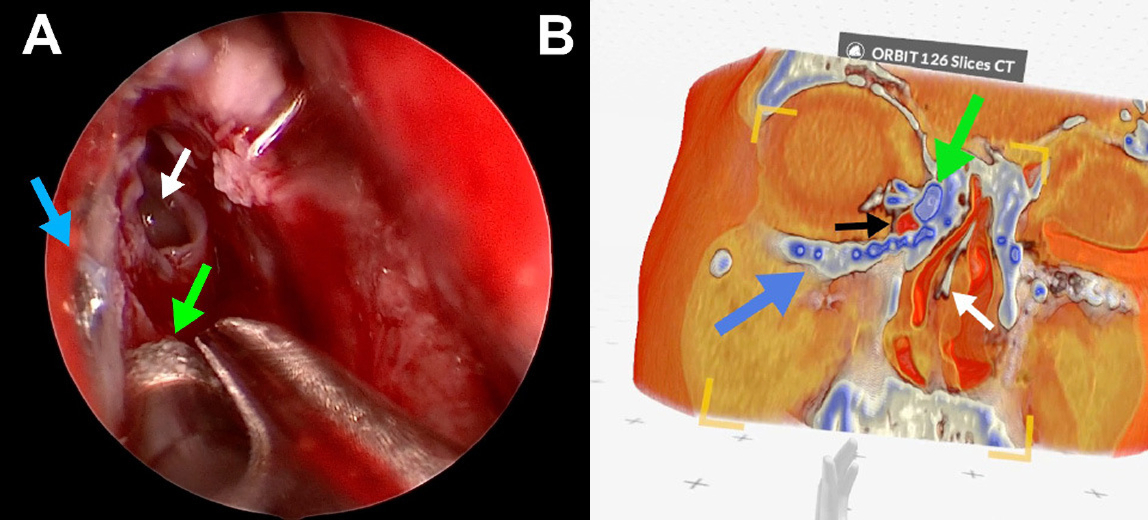
Panel A: 2D platform with tumoral voxel contouring based on DICOM imaging data. Panel B: 3D overview of tumor contouring of a cT4a gingivomandibular carcinoma.
Head and neck vascular planning
Vascular assessment and planning are essential in head and neck oncology, especially in patients with locoregional recurrence who may require multiple surgeries and free flap reconstructions. Conventional 2D imaging often fails to clearly depict existing vascular pedicles and territories. Immersive 3D imaging in VR enhances spatial understanding of vascular anatomy, supporting surgeons in selecting the most optimal surgical approach and identifying target vessels in advance. This helps reduce the risk of vascular injury and bleeding in previously irradiated or operated tissues.
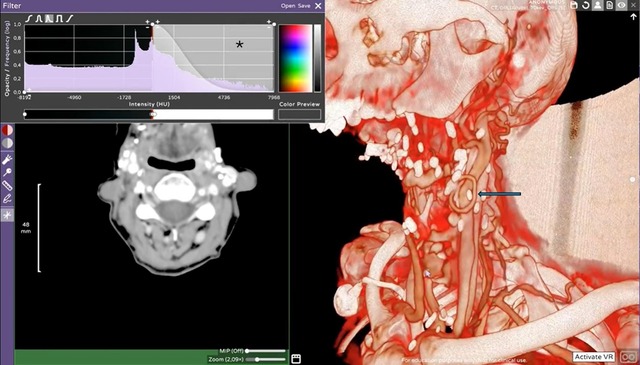
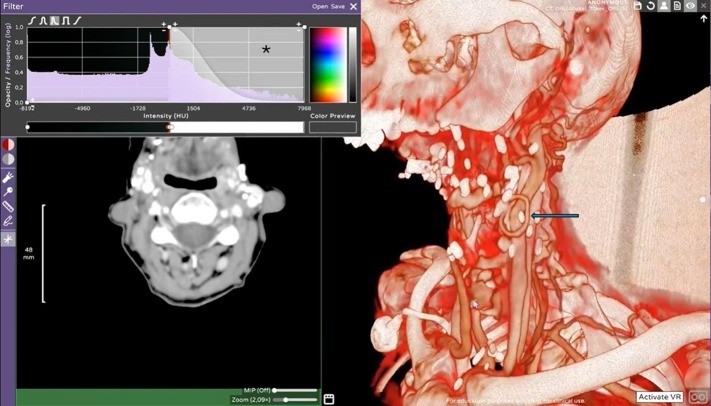
3D vascular planning of a patient with history of multiple mandibular surgical resection with a failed fibular free flap on left side with a fibular arterial loop over the external carotid branch and represented with the blue array. The asterisk indicates the Hounsfield unit window setting used to select the best parameters for the 3D overview.
Decision making
Decision-making in tumor boards involves complex multidisciplinary collaboration and traditionally relies on individual experience and two-dimensional imaging. These limitations may restrict shared understanding among team members. Integrating virtual reality into tumor board decision-making improves collaborative evaluation and clinical insight.
VR integration enables participants to visualize complex medical images and anatomical structures within a shared virtual environment. This increases understanding of the clinical situation, as well as communication and coordination among team members, oncologist, surgeon, radiologist and radiotherapist.
Immersive 3D tools strengthen both education and collaboration, helping experienced and junior clinicians better understand the therapeutic limitations and possibilities of each treatment option.
Future implementations
Using a 3D medical visualization platform with CT-scan reconstructions offers several advantages, including a high number of slices and contrast-enhanced imaging, which enables dynamic visualization of arterial and venous vascular structures. It also provides accurate representation of facial anatomy and bone structures. However, soft tissue–tumor contrast remains limited, making tumor delineation more challenging.
Future implementations of VR should focus on embracing both education and treatment, paving the way for a more interactive and immersive approach to healthcare.
For more information, contact info@medicalholodeck.com March 2026