Impact of Virtual Reality on Transcatheter Aortic Valve Implantation: A Prospective Randomized Controlled Trial. Circulation: Cardiovascular Imaging, 19, e018922.
https://doi.org/10.1161/CIRCIMAGING.125.018922Virtual Reality in cardiac surgery
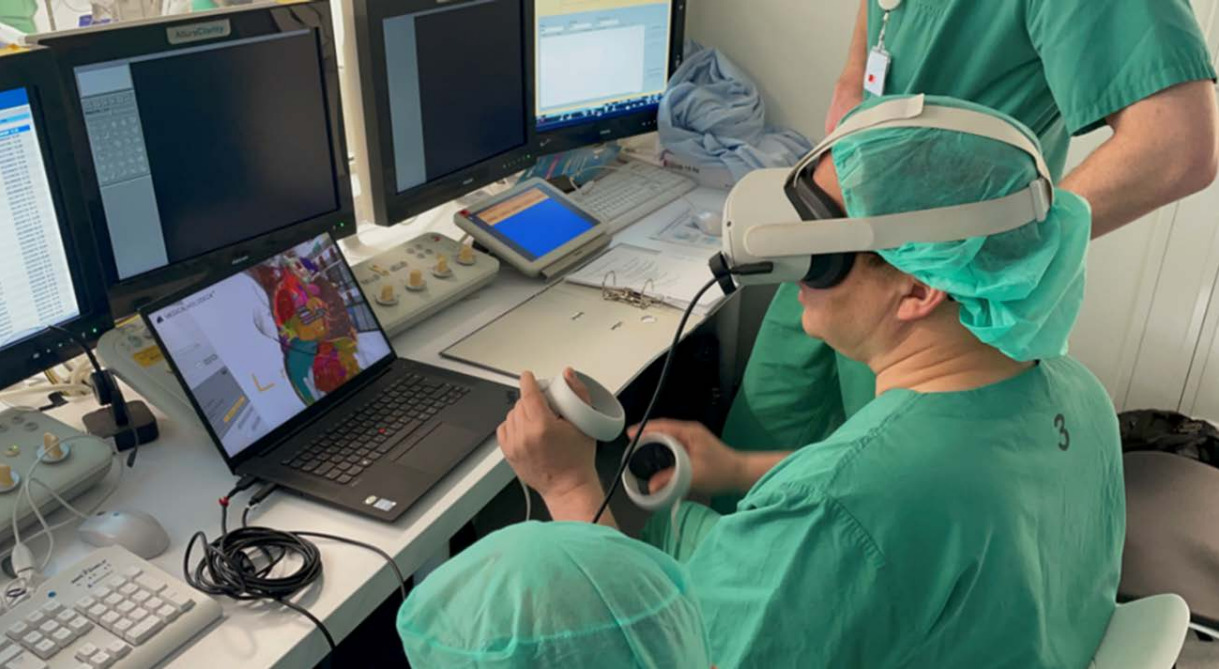
VR provides an immersive, interactive environment where clinicians can view and manipulate detailed 3D models of the heart and blood vessels. It improves spatial understanding and helps identify vessel pathways more effectively than 2D imaging.
Standard vs VR-supported planning
In this prospective study, 140 patients were divided into two groups. In the control group, preprocedural planning was performed using the 3mensio software alone for conventional flat-screen imaging. In the intervention group, planning was supported by Medical Imaging from Medicalholodeck, enabling visualization of patient data in an immersive 3D environment.
The use of both tools was evaluated using questionnaires, and procedural data and patient outcomes were compared between the groups.
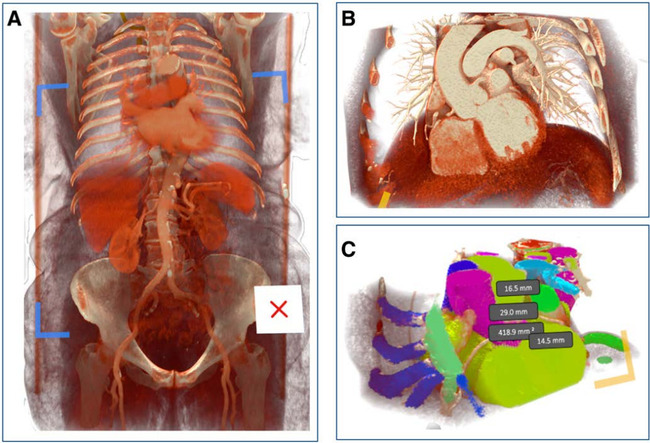
Advantages of VR-supported planning
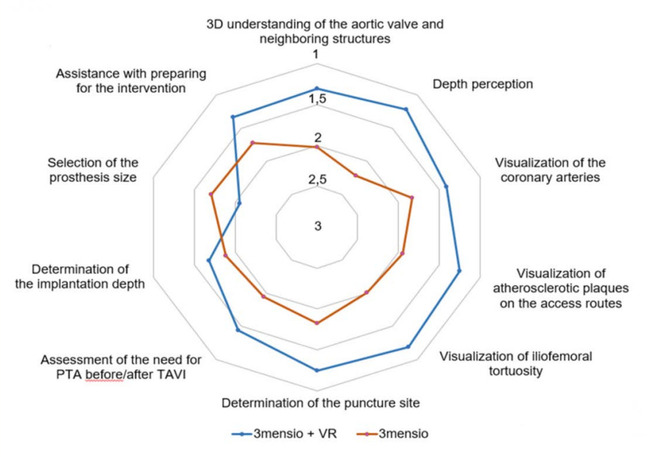
Virtual reality showed clear advantages over flat-screen imaging in helping clinicians understand complex anatomy. It improved perception of 3D relationships and depth, and provided better visualization of vascular access routes, including atherosclerotic plaques, vessel tortuosity, and optimal puncture sites.
While both methods were considered useful for procedural planning, VR offered a more intuitive and detailed understanding of anatomical structures.
Better patient outcomes
VR offers a more intuitive, 3D way to view these structures, helping clinicians choose the best puncture site and access route. As a result, the VR group experienced a lower rate of access-site bleeding. Other complications were similar between groups.
Importantly, there were no significant differences in procedural metrics, as VR did not increase procedure time, contrast usage, or overall complexity. In addition, the technology required only minimal training, supporting its practical implementation in clinical settings.
VR in surgical planning
Combining conventional imaging with advanced software and immersive visualization enables more tailored planning based on each patient’s anatomy. This approach has the potential to reduce complications, improve safety, and enhance overall outcomes. The findings from the University of Düsseldorf suggest that integrating VR into clinical workflows can support the optimization of TAVI procedures.
Try it yourself to see how immersive spatial imaging can support your clinical workflow. Download Medicalholodeck here.
For more information, contact info@medicalholodeck.com May 2026
